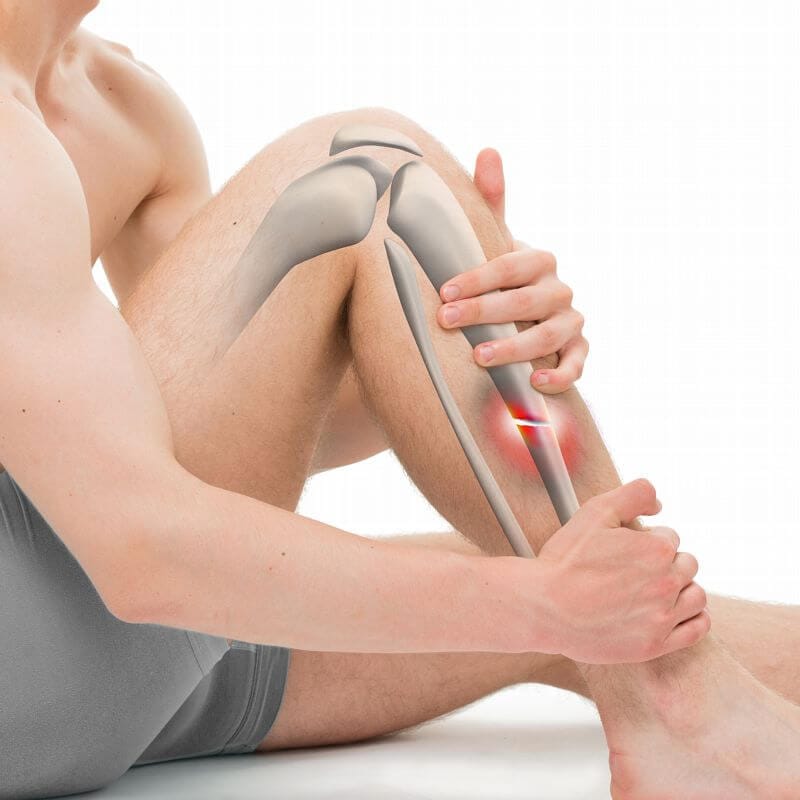
Fractures, commonly called broken bones, can present in various forms and necessitate prompt and precise management. Depending on the severity of the injury, the recovery period for a fracture can range from a few weeks to several months. It is essential to note that mild bone fractures often heal spontaneously, whereas severe fractures may require surgical intervention, immobilization, and the implementation of physiotherapy at various stages of recovery.
What Causes a Bone Fracture?
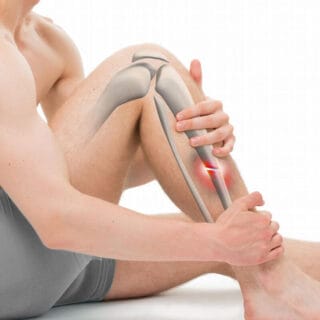
Bone fractures typically result from traumatic incidents, including automobile accidents, falls from height, and slips leading to awkward landings. The underlying cause of a fracture is generally evident. Moreover, stress fractures can arise from repetitive physical activities, manifesting as hairline fractures in weight-bearing bones, particularly the tibia in the lower leg. These fractures are frequently observed among athletes.
What Are the Types of Bone Fractures?
Bone fractures can be categorized into several distinct types:
1. Complete Fractures:
Characterized by the bone breaking into two or more separate fragments. These fractures can be further classified by their orientation—transverse, oblique, or longitudinal—and may also present as spiral or winding fractures.
2. Open Fractures (Compound Fractures):
These are complete breaks where the bone pierces the skin, resulting in a higher risk of infection. Such injuries require immediate medical attention.
3. Closed Fractures (Simple Fractures):
In this type, the integrity of the skin remains intact, and the bone does not protrude.
4. Incomplete Fractures:
These involve a crack in the bone without complete separation into two parts, with hairline fractures being a common example.
5. Displaced Fractures:
These complete fractures involve misaligned bone fragments, which often necessitate surgical intervention to realign for proper healing.
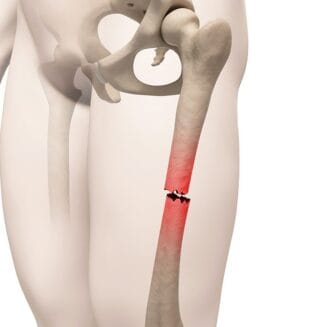
6. Comminuted Fractures:
A fracture in which the bone is shattered into several pieces, demands a complex surgical approach.
7. Greenstick Fractures:
These involve fractures that do not extend completely through the bone, which are primarily encountered in children due to the flexibility of their bones.
8. Buckle Fractures:
A specific type of greenstick fracture is where the bone bends without breaking completely.
9. Compression Fractures:
These occur when a bone collapses due to excessive pressure, frequently observed in individuals with degenerative spinal conditions.
10. Avulsion Fractures:
These occur when an injury causes significant tearing of muscle and ligament, resulting in a bone fracture.
It is important to acknowledge that while dislocations are not classified as fractures, they frequently occur concurrently with fractures in the event of a severe injury.
What Are the Symptoms of a Bone Fracture?
Individuals with bone fractures typically experience acute pain, and dizziness, and may exhibit nausea. The affected limb may be immobile and unable to bear weight. Other symptoms encompass a grinding sensation, bruising, swelling, tenderness, discolouration, and, in the case of open fractures, bleeding. Misalignment of the limb is a conspicuous indicator, particularly in instances of complete fractures.
Who Is at Risk of Bone Fractures?
Although all individuals are susceptible to bone fractures, certain populations are at heightened risk:
Older Adults:
Many individuals over the age of 50 demonstrate symptoms of osteoporosis, leading to thinner and more fragile bones. Approximately 50% of women and 20% of men sustain a fracture after the age of 50.
Post-Menopausal Women:
The reduction of estrogen levels significantly increases the risk of developing osteoporosis.
Athletes and Dancers:
Participants in contact sports such as hockey and football are at risk of various fracture types, including open fractures. In addition, non-contact sports may lead to stress fractures, while extreme sports such as horseback riding, cycling, and skiing pose risks for severe injuries. These individuals must wear appropriate protective gear.
Individuals with Chronic Health Conditions:
Those with chronic illnesses, including diabetes, osteomyelitis, rheumatoid arthritis, ongoing infections, and cancers that metastasize to the bones, are more vulnerable to fractures.
Individuals With Poor Lifestyle Choices:
A diet deficient in essential vitamins and minerals elevates the risk of osteoporosis. Regular physical activity is essential, and a diverse exercise routine is critical in preventing stress fractures. Maintaining proper nutrition, engaging in consistent exercise, and ensuring adequate sunlight exposure for vitamin D synthesis are fundamental preventive measures.
Children:
Due to their developing bones and greater flexibility, children are particularly susceptible to greenstick and buckle fractures.
What to Do If Someone Has a Bone Fracture
In cases of suspected skull fractures, compound fractures, or other serious injuries, it is imperative to seek emergency medical assistance without delay. Do not attempt to move the injured individual or create a splint; such actions should be conducted by qualified medical professionals. Timely medical intervention is crucial to achieving effective treatment and optimal recovery outcomes.